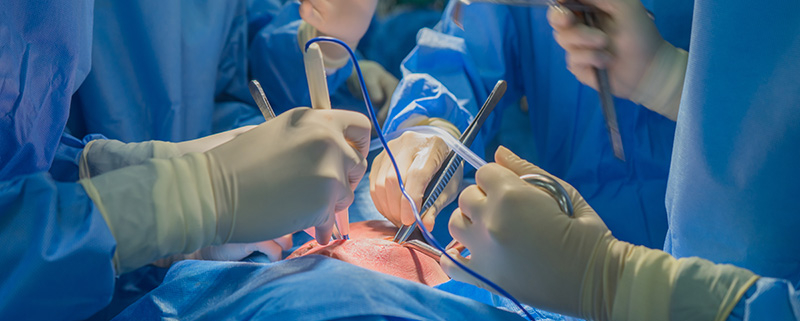
Most people only ever face the question of whether to become an organ donor when they renew their driver’s licence. A few confront it when close relatives suffer kidney failure. Hardly anybody decides they have excess kidneys and volunteers to donate one to a needy stranger. Nick Schwarz shares some guidance on the ethics of organ donation by living donors and by donors immediately after their death.
In wealthy countries with advanced health care systems like Australia and New Zealand, people who suffer organ failure often go on a waiting list for a transplant. They rely on an organ coming from someone else – an organ donor.
There is a waiting list because there are always more people who need transplants than there are suitable organs available.
Organs can be taken from the bodies of people immediately after their death, or, in the case of kidneys, they can be donated by living people, as most people are born with two functioning kidneys. A healthy person can function well on one kidney if the other is removed.
Australia deals with the shortage of donor organs by allocating available organs fairly, and by encouraging drivers to tick the organ donor box on their licence which consents to organ donation after their death.
IT’S PERSONAL
Imagine your brother or sister needs a kidney transplant. As a healthy person with two normal kidneys, you might consider offering one of yours! Being closely related genetically means your sibling’s body has a better chance of accepting your kidney.
If you did offer one, and your sibling agreed (and you passed all the necessary screening), you’d have an operation to remove one of your kidneys for immediate transplant into your sibling. You’d most likely recover from the surgery in about eight weeks but face potential complications in the days after the operation such as bleeding, wound infection and pneumonia. In the long-term, you should be able to lead a relatively normal life, aside from avoiding contact sport to protect your remaining kidney. Your gift will dramatically enhance your sibling’s life expectancy and quality of life.
Choosing to donate a kidney while still alive is a big deal. Because it is ethically complicated, there is no campaign to encourage it. Living organ donation goes against the traditional ‘do no harm’ principle in medicine because it involves healthy individuals undergoing medical interventions that are not for their own benefit and which cause short-term pain with no long-term gain.
Potential donors are assessed for their suitability and have the short and long-term risks and consequences explained to them. In Australia and New Zealand, the choice to donate a kidney is supposed to be voluntary. Nobody is supposed to be pressured into it. It is also meant to be a gift, with no payment involved or special conditions attached.
WHAT ABOUT VITAL ORGANS LIKE YOUR HEART?
The ‘dead donor rule’ states that doctors can only take vital organs like the heart, lungs and liver from people who have died. Even if it would improve the chances of a successful transplant, it is unethical to ‘finish off’ (i.e. murder) dying patients to ensure organs are as fresh as possible. To avoid perceptions of a conflict of interest, separate medical teams deal with (a) the business of treating the dying and confirming death, and (b) the business of harvesting and transplanting organs.
For many families of organ donors, coming to terms with their loved ones’ death is complicated by the need to understand and accept the concept of ‘brain death’. Brain death occurs when, because of an injury or accident, the whole of a person’s brain is deprived of oxygen for so long it permanently stops functioning. Patients diagnosed as brain dead can still appear to their families to be alive because artificial life support is used to pump air into their lungs to oxygenate their blood and keep their heart going and their skin warm and of normal colour. Without proper explanations and support, they can be traumatised by the misapprehension that their loved one is still alive as, still attached to life support, they are taken away to an operating theatre to have their organs removed and given to unknown recipients.
DIFFERENT COUNTRIES, DIFFERENT POLICIES
In Australia and New Zealand, we have an ‘opt-in’ organ donation policy. This means organs can only be removed from people who have explicitly stated that they want to be an organ donor. The wishes of families are respected, however. Organ donation can’t proceed without the family’s agreement. Opt-in organ donation is the norm in English-speaking countries where we have a strong sense of ownership over our bodies and want a say over what happens to them even after we are dead.
Some countries such as Spain, France, Norway and Sweden have an ‘opt-out’ policy. There, adults must explicitly state they don’t want to be an organ donor, or they’ll be presumed to have consented to being one. The wishes of families are still taken into account, however. If families say no, donation won’t proceed.
The citizens of Iran can legally buy and sell kidneys in a government-regulated trading system. But in Iran and many other nations around the world, there is also illegal trading in organs. ‘Transplant tourism’ occurs especially in China, India and Pakistan, where medical services are sophisticated enough to perform transplant surgery for rich locals and foreigners.
Organ traders prey upon the poor for cash in exchange for kidneys, then sell them at a profit to transplant clinics. Kidneys and other organs are also reportedly harvested from prisoners and people who are kidnapped and murdered, including homeless people, people with unpaid debts and dissidents.
See the more information reference for details about the ethical principles that underpin Australia’s and New Zealand’s current organ donation policies.
A CHRISTIAN PERSPECTIVE
God’s clearest source of his will for us, the Bible, offers no clear directions for us on organ donation. That’s no surprise given it was written many centuries before organ transplantation became possible. Even so, God’s word is still helpful.
The Bible teaches that human life is precious. God himself creates and gives life to every human being. Most churches consider Jesus’ life and teachings as neutral on or leaning towards support for organ donation. Those that believe they find support in the Bible cite evidence like the following:
- Jesus modelled sacrificial love. He invites us to follow his example, saying, ‘Love one another as I have loved you’.
- As Jesus sent out his disciples, he instructed them to, ‘Heal the sick… freely you have received, freely give’ (Matthew 10:8).
- Jesus healed the sick. He didn’t tell them their sickness was ‘God’s will’ or ‘God’s just punishment for sin’. He generously gave them a new lease on life.
- In Jesus’ Parable of the Good Samaritan (Luke 10:25–37), he urges us to extend our love and charity to neighbours in need.
Many Christians view organ donation as ‘acceptable’ or ‘good’ and willingly register as organ donors provided it occurs in a way that is consistent with Christian ethics. If the circumstances of their death were to open up the possibility of organ donation, they would be pleased to honour God’s gift of life by giving to others a new lease on life. Key criteria for Christian support are that:
- the donor and their family consent,
- the donor is dead when vital organs are removed,
- it is done in a way that treats the body of the donor with respect,
- it treats the family of the donor with respect and compassion,
- it is truthful, respectful and fair towards organ recipients, and
- organs are donated freely and unconditionally.
Yet Christians who support organ donation on these terms will also be slow to criticise individuals who cannot bring themselves to say yes, or families who override a recently deceased loved one’s wishes to donate their organs. The lack of clear biblical teaching on organ donation should caution us from being judgemental.
TALK ABOUT IT WITH YOUR FAMILY
Discuss your thoughts on becoming an organ donor with your family. If you end up in a situation where your organs might be removed for transplantation, your family will need to give consent – right when they are trying to process the news that you are dead. It will be a very difficult time for them and talking with them in advance will help not to add to their trauma.
Current policy allows the family to refuse permission for organ donation. If you wish to donate your organs but your family is opposed, you’ll need to convince them they’ll be able to give permission and feel sure they have done the right thing.
A good time to review your decision about becoming an organ donor and talking with your family about it is when your driver’s licence is renewed. Check that organ donation and transplantation are still being done in a way that aligns with Christian ethics and discuss organ donation again with your family.
Nick Schwarz is the LCANZ’s Assistant to the Bishop – Public Theology and a consultant to the church’s Commission on Social and Bioethical Questions (CSBQ). His Christian ethical decision-making guides are available at www.lca.org.au/csbq
For more information, go to the Australian Government Organ and Tissue Authority: www.donatelife.gov.au and click on the ‘All about donation’ tab.